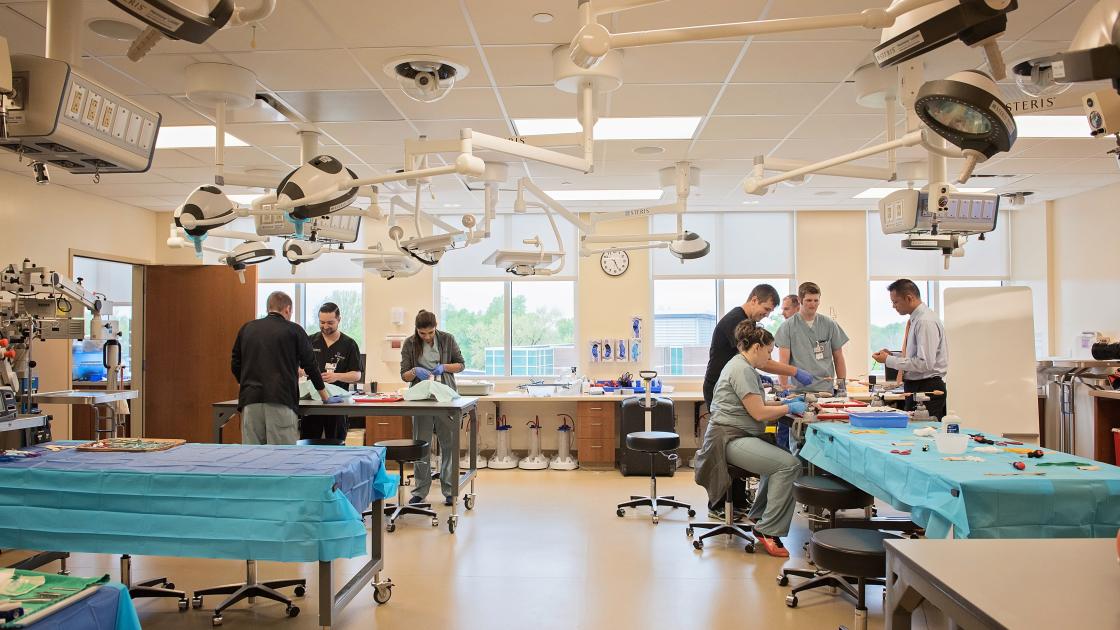
Surgical Skills Center
The orthopedic surgery residents were crowded around tables of the J. Roland Folse, MD Surgical Skills Center on the fourth floor of the Memorial Center for Learning and Innovation. Surgical equipment hummed as the doctors drilled and sawed into assorted pieces of resin. The materials were crafted to create realistic resistance for the surgical residents as they practiced the procedures over and over, perforating and precisely removing sections from the blocks and cylinders.
And there was another thing removed from the surgical simulation: the heightened pressure a trainee would experience in an operating room. This lower-anxiety setting is why the surgical skills center has become one of SIU School of Medicine’s most popular training destinations.
It was championed by a forward-looking SIU surgeon who envisioned a versatile facility where surgeons could practice and proficiency would prevail.
BUILDING CONFIDENCE
Gary Dunnington, MD, former professor and chair of the SIU Department of Surgery and founding director of the SIU Surgical Skills Lab, led the efforts to open the Springfield-based Surgical Skills Lab in May 2000. At the time, it was one of the nation’s only laboratories designed specifically for training surgical residents.
Skills labs have since revolutionized surgical training. Using computer simulators and virtual reality technology, as well as specially designed procedure models, surgical residents learn a wide array of skills including instrument tying, one/two-handed knot tying, laparoscopic procedures, vascular anastomosis, chest tubes, central lines and splinting.
Dunnington and the surgical faculty and staff had helped create the national curriculum developed jointly by the American College of Surgeons and the Association of Program Directors in Surgery, comprised of three phases. Phase 1 and 2 includes modules that address basic surgical skills, designed with first- and second-year residents in mind.
Janet Ketchum has been the surgical skills director and skills coach in the Department of Surgery since the center opened in 2000. She was working in Memorial Medical Center’s operating room as a scrub nurse and preceptor for the new nurses when Dunnington recognized her aptitude as an educator.
With a $50,000 private grant and some generously donated space adjacent to Memorial’s OR, Dunnington asked Ketchum to join him in creating the Surgical Skills Center.
The center was established to address the increasing complexity of surgical techniques in a reduced-stress environment, free from patient safety concerns. Its simulationdriven skill labs were an immediate hit with general surgery residents, and sessions were soon expanded to include other specialties: urology, plastics and orthopedics. An open-door policy allowed learners to practice procedures in their spare time.
The confines were intimate and sometimes got crowded, Ketchum said, even after Memorial enlarged the space. Storage was always at a premium because specialized surgical instruments were needed as technologies evolved.
The medical school does not keep its successes secret. In its formative years, Dunnington and the staff organized and hosted annual two-day CME workshops on the basics of setting up these unique teaching spaces, to help dismantle hurdles before they appear.
In 2013, planning for the Memorial Center for Learning and Innovation was getting underway. The $40-million, four-story facility would be built on property adjacent to both Memorial Medical Center and SIU School of Medicine. The plans designated a spacious wing of the top floor for a new Surgical Skills Center.
The new J. Roland Folse, MD Surgical Skills Center was dedicated in August 2015, named in honor of SIU’s first chair of the Department of Surgery
SIU surgeons value the time spent in the state-of-the-art facility with their teams. Rebecka Lopez, MD, assistant professor in the Department of Emergency Medicine, said, “The skills center gives our residents some of the best opportunities to hone their skills with the safety net of simulated models and direct, hands24 WINTER 2019 | ASPECTS on instruction. They can experience some once-in-a-career procedures before ever having the life of an actual patient on the line – an encounter that can be truly life-saving in the future.”
“When I visit other centers, I often see skills labs that are ‘expensive closets’ in the sense that they have nice equipment, but are empty most of the time,” said Dr. John Mellinger, professor and chair of the Division of General Surgery. “Residents are encouraged to use them, but are on their own to do so, and rarely able to amidst other duties.”
“The beauty of our facility is not just the physical space, but the curricular, staffing and protected time for use strategies that make the lab hum with learner activity on a daily basis.”
MODEL MAKING
Senior skills specialist Jennifer Bartlett is the engineer responsible for creating many of the lab simulation models. There are realistic hands, fingers and toes cast in poured silicone from alginate molds and an impressive array of unique molds and models, many fashioned in MacGuyver-like simplicity. Models typically fit into two categories: things surgeons encounter all the time or “specialty items.” The latter are as important as the former, because no surgeon wants to be unfamiliar with something that a patient is experiencing.
Novelty pushes research forward, so when Bartlett creates a specialty item, she frequently designs ‘how-to’ documentation around it that the physician can integrate into a research article. The Surgical Skills team freely shares its construction processes with colleagues and other medical schools.
Bartlett and skills specialist Brian Hollinshead have attended classes to expand the center’s repertoire. After a recent workshop where they learned how to mold an entire head, an SIU plastic surgeon contacted them to do just that. The surgical team already had a template of the bony part of the subject’s face but wanted a cast of the soft tissues so they could prepare scenarios for the reconstruction process.
Because she’d never done a whole-head cast, especially one so crucial to a surgical team’s plan, Bartlett contacted the workshop hosts and explained the situation. “They were able to send a professional to Springfield who cast the patient’s head in the doctor’s office,” she said. The resulting mold was then used to try multiple approaches for the best possible surgical outcome.
The surgical skills team is eager to add a state-of-the-art 3D printer to their service line. Ketchum envisions using it for mass-production of the more sophisticated models that require different textures. It could also be engineered for one of the group’s newest assignments. Dr. Matt Johnson, assistant professor in the Department of Otolaryngology-ENT, has asked Bartlett to create a soft tissue face mold for cleft palate repair. The procedure is one of the most frequently performed surgeries on mission trips. The models could be sent overseas in advance for physician training and remain behind after the mission’s ends to help sustain the quality of the work.
With two decades of experience to draw upon, the Surgical Skills Center will continue to refine its technology and teamwork to meet the next anatomical challenge, to improve training opportunities and to enhance the abilities of SIU’s students, residents and surgeons.





