Limbs Back to Life
SIU vascular surgery helps patients overcome pain and disability with thoracic outlet decompression surgery
Written by Rebecca Budde • Photography by Jason Johnson Aspects Winter 2015, Vol 38-1.
Annalese Corwin, 24, waited a year to be able pick up her five-year-old son, Carter, and give him the hugs he longed for or even push him on the swings at the park. "He was always asking me to take him to the park and push him on the swings, but I just couldn’t do it," she says. The pain in Corwin’s left shoulder, her dominant side, was so deep and the numbness in her arm was so unpredictable that these simple pleasures were impossible for her.
The pain stemmed from a 2013 car accident. Corwin found her left arm lifeless, falling to her side as she tried to brush her teeth or fix her hair. Numerous visits to her primary care physician and some physical therapy offered no relief. "I was prescribed muscle relaxers and pain medication. They made me so tired, I couldn’t take care of Carter," Corwin says. About six months after her accident, a referral to Jacob Monsavias, physician assistant in SIU’s division of orthopaedic surgery, finally started to turn things around for her. An MRI and nerve conduction study showed that the cause of Corwin’s pain was not a musculoskeletal problem. She had thoracic outlet syndrome (TOS).
Just behind and below the collarbone is a tiny space that causes massive pain for many people. The thoracic outlet houses the many blood vessels, muscles and nerves that serve the entire arm. "The nerves and veins have to make it through three different muscles, the rib and the clavicle; the space can be really tight sometimes," Sapan Desai, MD, PhD, MBA, explains. Pressure against the nerves or blood vessels in this area can cause debilitating symptoms.
Dr. Desai, assistant professor of vascular surgery, is one of the only physicians in Springfield who routinely performs thoracic outlet decompression surgery. This surgery is the only known cure for patients who suffer from TOS.
Symptoms of TOS vary based on the structure affected in that tiny space —nerves, veins or arteries. Neurogenic TOS, which is the most common type, can cause pain, numbness, neck pain, headaches in the back of the head, tingling and/or weakness in the affected arm and hand. Patients who have venous TOS usually have swelling in the entire arm plus pain and dark discoloration. Patients with arterial TOS, the rarest but probably the most serious of the three, present with pain, coldness, paleness and cramps when using their hand.
"I felt like I was getting nowhere and people didn’t believe me or think it was a serious problem. When I was finally diagnosed with TOS, it was a relief." - Annalese Corwin
"Many of those who suffer from TOS tend to be young, otherwise healthy individuals," Dr. Desai says. Repetitive stress injuries (RSI) and accidents tend to be the main cause of TOS, but habitual sleeping or working positions can also lead to TOS over time. "A painter, linesman, hairdresser, pro athlete or someone who continually reaches overhead and does the same repetitive motion every day is more likely to develop TOS."
Tristen Karrick, 16, was one of those young, healthy individuals with a RSI. He woke one morning with a severely swollen arm. A color guard for his high school band, Tristen previously had intermittent fatigue, numbness and occasional swelling in his arm over a period of months, but the symptoms always resolved within a day or two. A venogram, an x-ray that takes images of the blood flow through the veins, showed that the blood flow in one of his major veins stopped where the clavicle met the first rib, indicating that the space was too tight for proper blood flow. "Tristen basically did the same motion over and over again as a color guard, leading to muscle hypertrophy, which tightened the space between his first rib and clavicle."
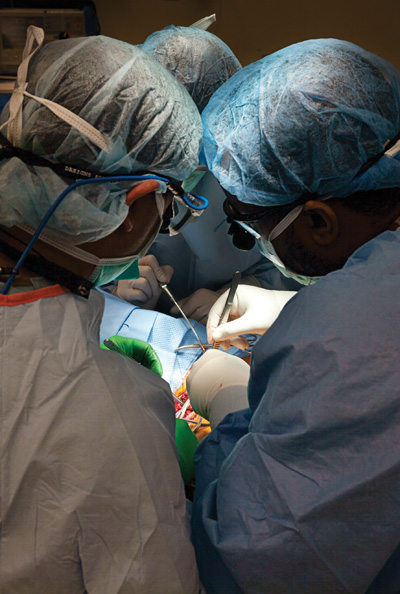 Left Image Caption: Dr. Desai and Dr. Jason Andre, PGY4, perform TOS surgery on Tristen Karrick.
Left Image Caption: Dr. Desai and Dr. Jason Andre, PGY4, perform TOS surgery on Tristen Karrick.
"If your muscles swell to double their size, there’s no room for anything to get through," Dr. Desai explains. "The veins and arteries can stop working, resulting in swelling in the arm and hand. The veins can clot, and you could actually lose your arm or the clots can travel to the lung and heart and create life-threatening pulmonary embolisms."
According to Dr. Desai, TOS is one of the most misdiagnosed or underdiagnosed diseases; his first patient went undiagnosed for 10 years. The vague symptoms can be confused with other conditions and lead to unnecessary surgeries and expensive therapies. "I felt like I was getting nowhere and people didn’t believe me or think it was a serious problem," Corwin says. "When I was finally diagnosed with TOS, it was a relief."
In some cases, physical therapy can somewhat improve the symptoms of neurogenic TOS. Physical therapy loosened up the muscles in Corwin’s neck to slightly improve her range of motion, but the pain and tingling never went away. Dr. Desai says that he requires patients with this type of TOS try physical therapy before considering an operation. By stretching the muscles in the neck, correcting posture and avoiding certain movements that may aggravate the symptoms, a few patients may find some relief. However, for most patients, the symptoms will continue or worsen, making TOS decompression surgery the best option for a cure.
"For those with venous or arterial TOS like Tristen, surgery is the best option," Dr. Desai says. "Some physicians will treat venous TOS with a stent, but that’s probably the worst thing to do. It doesn’t fix the problem. The stent will occlude, and when they come see me, I’ll have to do a bypass around the stent to fix the problem." Tristen Karrick underwent surgery in November.
Though she had a different type of TOS, surgery was the best option for Corwin too. "I was terrified, but Dr. Desai was amazing at explaining everything," she says. "Looking back, I’m so glad I didn’t wait to have the surgery. I never thought a car accident could cause something like this."
Whether its neurogenic, venous or arterial, TOS decompression surgery is tedious and lengthy. With the help of a dedicated surgery team and magnifying surgical loupes, Dr. Desai works carefully around the tangles of veins, muscles, nerves and arteries. For 3-8 hours Dr. Desai and a fourth-year resident work in tandem, heads occasionally touching. By making two incisions, one above the collarbone and one below, the surgeon removes the defective scalene muscles, the first rib if it is causing problems and sometimes scar tissue that can be extremely thick.
"It’s a lot of surgery for such a small area," says Dr. Desai, who received his training in TOS decompression surgery while at the Texas Medical Center and Duke University. Patients typically stay in the hospital for two to five days until they are able to get up and walk around on their own, eat well and manage their pain. Patients usually need some physical therapy after surgery.
Both Karrick’s and Corwin’s surgeries were successful. After a short hospital stay and physical therapy, Corwin returned home to her family. She continues physical therapy at home to regain strength and range of motion in her arm and shoulder. Her pain is gone. Karrick will begin the new year without any restrictions on using his arm. "He can go back to being a regular 16-year-old kid again and participate in color guard again soon." Dr. Desai says.
About a month after her surgery, Carter and Corwin took a trip to LEGOLAND® for Carter’s fifth birthday. "He had so much fun on that trip," she says. "And one of the best things was that I could finally lift him up to see things better. I wouldn’t have been able to do that before the surgery."
