ACGME core competencies
In September 1999, the ACGME developed minimum program requirements regarding education. They state in their mission, "The residency program must require its residents to obtain competencies in the six areas below to the level expected of a new practitioner. This section reviews in detail those competencies, how they are measured and when they are implemented. Detailed information can be retrieved from their website.
Programs must define the specific knowledge, skills and attitudes required and provide educational experiences as needed in order for their residents to demonstrate the following:
Residents must be able to provide patient care that is compassionate, appropriate, and effective for the treatment of health problems and the promotion of health.
Residents must demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social-behavioral sciences, as well as the application of this knowledge to patient care.
Residents must demonstrate the ability to investigate and evaluation their care of patients, to appraise and assimilate scientific evidence, and to continuously improve patient care based on constant self-evaluation and lifelong learning. Residents are expected to develop skills and habits to be able to meet the following goals:
- Identify strengths, deficiencies, and limits in one’s knowledge and expertise;
- Set learning and improvement goals;
- Identify and perform appropriate learning activities;
- Systematically analyze practice using quality improvement methods, and implement changes with the goal of practice improvement;
- Incorporate formative evaluation feedback into daily practice;
- Locate, appraise, and assimilate evidence from scientific studies related to their patients’ health problems;
- Use information technology to optimize learning; and, participate in the education of patients, families, students, residents and other health professionals.
Residents must demonstrate interpersonal and communication skills that result in the effective exchange of information and collaboration with patients, their families, and health professionals. Residents are expected to:
- Communicate effectively with patients, families, and the public, as appropriate, across a broad range of socioeconomic and cultural backgrounds;
- Communicate effectively with physicians, other health professionals, and health related agencies;
- Work effectively as a member leader of a health care team or other professional group;
- Act in a consultative role to other physicians and health professionals; and,
- Maintain comprehensive, timely, and legible medical records, if applicable.
Residents must demonstrate a commitment to carrying out professional responsibilities and an adherence to ethical principles. Residents are expected to demonstrate:
- Compassion, integrity, and respect for others;
- Responsiveness to patient needs that supersedes self-interest;
- Respect for patient privacy and autonomy;
- Accountability to patients, society and the profession; and,
- Sensitivity and responsiveness to a diverse patient population, including but not limited to diversity in gender, age, culture, race, religion, disabilities, and sexual orientation.
Residents must demonstrate an awareness of and responsiveness to the larger context and system of health care, as well as the ability to call effectively on other resources in the system to provide optimal health care. Residents are expected to:
- Work effectively in various health care delivery settings and systems relevant to their clinical specialty;
- Coordinate patient care within the health care system relevant to their clinical specialty;
- Incorporate considerations of cost awareness and risk-benefit analysis in patient and/or population-based care as appropriate;
- Advocate for quality patient care and optimal patient care systems;
- Work in inter-professional teams to enhance patient safety and improve patient care quality; participate in identifying system errors and implementing potential systems solutions.
The Resident Case Log System can be selected in this system to view information regarding entry of information, etc. All residents are expected to be assessed by the guidelines established by the ACGME.
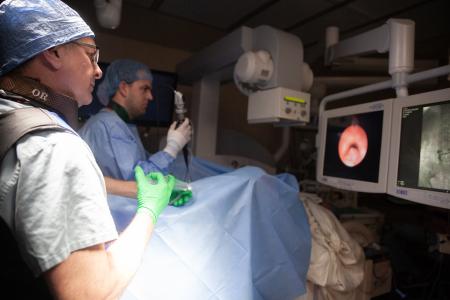

Resident duties
During the course of the urology residency program, the individual resident will have a variety of responsibilities including, but not limited to, patient care, preparation for conferences, teaching, and research. Each responsibility will be shared with other individuals including fellow residents, urology faculty, attending physicians and surgeons from other services. The individual urology resident should always initiate communication between the chief resident in urology and the faculty to assure that involvement and input from all responsible parties is maintained.
In-service exams provide the faculty with information about cognitive advancement in comparison to peers. Residents' participation is mandatory and exceeding 50 percentile of peer group is required. Failure to do so may result in academic probation, suspension of operating room privileges, withdrawal from national, regional or local meetings, or other remediation as determined by the faculty. Mock oral and written exams are administered in addition to the formal in-service exam given in the fall of each year.
Residents will complete two rotations while in their PGY2-5 years. The first service covers HSHS St. John's Hospital and SIU Outpatient clinics. Residents will cover all SIU inpatients at this hospital and all surgical cases. Residents will be exposed to all urologic subspecialties, including pediatrics, during rotations. Multiple DaVinci Robots are available at this hospital with teaching consoles and simulators to aid in education. New and innovative surgical devices are available at St John's including Rezum and Thulium lasers. The second rotation is at Springfield Memorial Hospital. Residents on this rotation will cover all SIU inpatients at this hospital. All subspecialties of urology except for pediatrics are represented by the surgeries conducted at Springfield Memorial Hospital. Multiple DaVinci robots are available with teaching consoles and simulators to aid education. Thulium, high-watt holmium and UroLift devices are all available at this location. Duties and cases covered at both hospitals by the residents will be commensurate with the level of training and education.
Residents will cover all SIU inpatients at this hospital and all surgical cases. Residents will be exposed to all urologic subspecialties, including pediatrics, during rotations. Multiple DaVinci Robots are available at this hospital with teaching consoles and simulators to aid in education. New and innovative surgical devices are available at St John's including Rezum and Thulium lasers. The second rotation is at Springfield Memorial Hospital. Residents on this rotation will cover all SIU inpatients at this hospital. All subspecialties of urology except for pediatrics are represented by the surgeries conducted at Springfield Memorial Hospital. Multiple DaVinci robots are available with teaching consoles and simulators to aid education. Thulium, high-watt holmium and UroLift devices are all available at this location. Duties and cases covered at both hospitals by the residents will be commensurate with the level of training and education.
The outpatient clinical experience in which patients are evaluated and managed is necessary for residency training and accreditation and is a key element of urology training. The resident outpatient experience will be one in which the residents are given appropriate responsibilities and an opportunity to make diagnostic and therapeutic decisions concerning the need for surgery. They will have the opportunity for continuity of care outside of the hospital for those patients who have had surgery.
Each resident will have their own personal half-day clinic every week under the supervision of a faculty member. This clinic includes experience in outpatient procedures such as cystoscopy and transrectal ultrasound-guided biopsy of the prostate. Each resident is responsible for the care of patients in their clinics, including promptness in attendance, evaluation and management of clinical problems, follow-up of laboratory and imaging studies, scheduling surgery and follow-up appointments and communication with referring physicians. Specific disease states can be discussed with the representative faculty specialist. Clinics will be organized in a way that residents will be able to follow their patients throughout their residency, giving them the opportunity to manage patients over an extended period of time. The faculty providing oversight may change but resident involvement will be consistent.
Call is shared among residents at about 1:4 although this varies depending on when interns are on service. Interns will typically join the call pool starting their second month of urology. Juniors take the primary calls with a senior or chief resident as back up to assist in seeing consults and covering emergent procedures. Emergency room and unassigned patient call is shared with a private practice group with a 50/50 split. Weekends are divided such to allow for two whole weekends off per month.
The resident is expected to be available when the patient is taken to the operating room. When the patient enters the operating room, the resident should be available to have all imaging readily available, to aid in proper positioning of the patient and to be present during induction of anesthesia. The resident should oversee the prepping and draping of the operating room. In addition, residents who participate as the operating surgeon should have chart documentation of participation and understanding of the preoperative workup.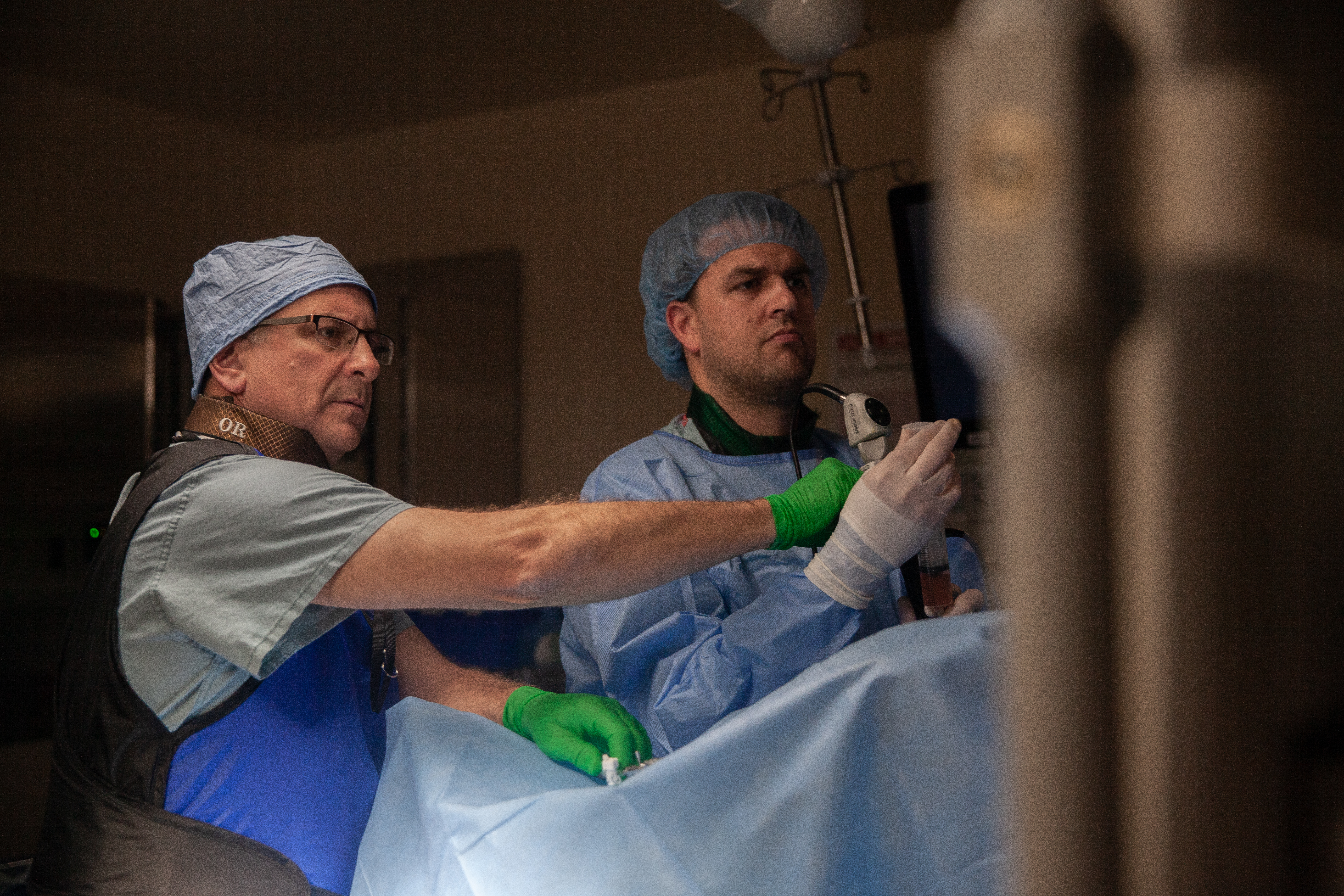
The chief resident has the option to choose cases on any of the services. Exceptions include resident clinic patients and faculty decisions. The resident assigned to a service where the chief resident is the operating surgeon will be present during the operation and will be responsible for the postoperative care. It is expected that the chief resident will be available to all of the residents for advice and help with the care of all patients, especially in those cases in which he or she served as the operating surgeon.
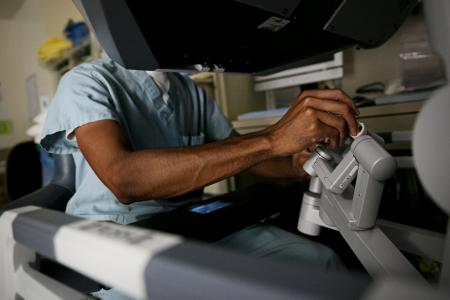
The residents will be participating in robotic surgery and will become competent in many robotic urologic procedures. As part of the robotic curriculum, residents will be required to create profiles and complete all simulation on the DaVinci robotic simulators prior to participating in robotic procedures. These simulators are located at both St. John's and Springfield Memorial Hospital and are readily available to all residents at all times.
The ACGME has established a required minimum number of cases in each of the index categories and procedures to maintain program accreditation. Therefore, it is important to maintain an accurate accounting of surgical cases. Residents at all levels are required to log their operative cases onto the ACGME website on a daily basis. Failure to do so may result in the suspension of operative room privileges.
Each resident is expected to participate in at least one SIU committee.

Conferences
A half-day each week is set aside for the urologic didactic conference. Attendance at the following meetings is mandatory and absence requires approval from the urology Program Director or Residency Program Coordinator. Each conference day varies but will consist of a variety of conferences.
Discussion of interesting cases from the prior week or near complications that will not be discussed in M&M conference are explored.
A weekly session in which residents discuss in length, a specific surgical procedure. This includes a detailed discussion of indications, complications, outcomes and the steps of the operation. Each aspect should be thoroughly researched and current literature cited during the presentation.
Each class of urologic pharmacology will be reviewed. The current urologic uses, side effects, cost, etc. will be discussed in detail with an emphasis on applicability to, and optimization of, current practice.
A review of interesting or unusual cases, highlighting diagnostic and treatment options/algorithms, pathophysiology and review of the literature surrounding the case.
AUA Guidelines/Best Practice Statements
The assigned resident uses new self-made questions to highlight the features of the AUA guidelines being reviewed. Questions are meant to clarify the details and act as reinforcement of the guidelines.
The Mortality and Morbidity Conference is critical for surgeons in training. The format is an in-depth analysis of significant morbidity or mortality with a literature review of specific complications. The resident who worked on a particular case will present the facts of the case and prepare an evidence-based discussion on the cause and prevention of the morbidity or mortality. The resident or faculty may be assigned a topic specific to morbidity and mortality. The resident or faculty is expected to provide copies of relevant journal articles for distribution to those participating in the conference. The full-time faculty or volunteer clinical faculty member involved in the case is expected to be present. A competency-based summary form must be completed and filed with the residency coordinator. Emphasis is placed on objective publications related to the case and systems-based problems and how they are corrected using the systems in place at the specific sites of service.
Presentations involving community faculty will be made during normal Wednesday morning conference time for routine complications with limited educational value.
M&M presentations for both academic and community faculty which are more complex, unusual or have greater educational value, will be presented to the combined group of attendings after the hospital Urology department meetings occurring on Monday afternoons/evenings on a quarterly basis.
A monthly conference attended by the urology division and representatives from pathology, radiology, medical oncology and radiation oncology is used as a forum to discuss complex urologic cancer cases and come up with consensus decisions on further diagnostic workup or treatment regimens.
Interesting and educational cases that have relevant radiographic imaging will be presented to the division for comment and learning. The resident who worked on a particular case will present the facts of the case and is responsible for presenting an evidence-based discussion of the relevant issues. This conference prepares the residents for the uroimaging portion of the American Board of Urology exam.
This conference is held in conjunction with the Department of Pathology at Springfield Memorial Hospital and St. John’s Hospital. The pathologists conduct conferences. The case selection is prepared jointly by Urology and the pathologists. This conference prepares residents for the uropathology portion of the American Board of Urology exam. Pathology is presented as an unknown with residents identifying the pathology. This is combined with a specific didactic session on different areas of urologic pathology.
Fourteen skills lab modules have been developed with the purpose of improving the residents' technical skills in areas such as Cysto/Ureteroscopy, Percutaneous Nephrolithotomy, Open & Laparoscopic Partial Nephrectomy, Urethral Injury Repair, Transurethral Resection of the Prostate, Laparoscopic Skill & DaVinci Robot Training, Introduction and Advanced Transurethral Endoscopy, Urethral Reimplant & Deflux Lab, Principles of ultrasound and advanced fluoroscopy and operating room imaging. Anatomy and cadaver labs provide additional training in fundamental aspects of urology. Both resident and faculty evaluations will be completed after the labs. Learn more: Visit the J. Roland Folse, MD. Surgical Skills Center.
This is a 4 hour surgical skills lab that utilizes animal models for demonstration, instruction and practice of microsurgical techniques. Individual, one-on-one training sessions with the senior level residents are required before they are allowed to participate in advanced microsurgical surgery. This lab can also be accessed for practice and improvement of personal microsurgical skills.
As part of our surgical skills curriculum, residents will be exposed to and have extensive work in all new and innovative forms of benign prostatic hyperplasia (BPH) treatment. This includes simulations available to the residents 24/7 within the MCLI surgical skills center, hands-on experience on cadaver and animal models and presentations from leaders in non-urologic options for this condition (specifically IR prostatic artery embolization). This allows the residents to be knowledgeable and experienced with all options for treating this common and debilitating condition to make the best recommendation for their future patients.
Every other month, the research endeavors of the urology division are discussed openly and critically. Presentations and talks to be given at local, regional, national and international conferences will be practiced during this time. Activities in the Urology Research Lab will also be disseminated. Papers for submission are reviewed and research assignments are reviewed and updated.
It is imperative that urologists in training understand the indications, complications and alternatives to all urologic procedures. This conference enables the resident to discuss pre-operative evaluations and surgical alternatives to urologic diseases. Residents are expected to propose treatments and be prepared to defend them against alternative therapies.
Journal Club meetings are held monthly. A faculty member assigns topics and articles for review. Each resident is assigned to critically review an article in the current or classical urologic literature. Open discussion following each presentation is encouraged to provide insight into the merit of the particular article and how it will change clinical practice. Survey articles from the Journal of Urology are reviewed every other month.
Additional educational curriculum sessions
Sleep deprivation and fatigue education is a required online module that every incoming resident must take before beginning work as a PGY-I resident. Sleep deprivation and fatigue are routinely monitored by faculty, chief residents and senior residents. All fatigue issues are addressed as they arise and fatigued residents are sent home for rest.
During PGY-I orientation, SIU Human Resources presents a sexual harassment lecture. This is supplemented by online modules required throughout the residency by the residents’ respective employing hospitals.
The introductory course is presented by Residency Affairs as an online module residents must complete before beginning work in their PGY-I year. More detailed and thorough sessions are given by the Department of Surgery in the PGY-II and PGY-IV years. Topics during these sessions include: The Art of Giving a Presentation, Departmental Expectations of Students on Surgery Clerkships, Strategies for Clinical Teaching, Teaching at the Bedside, Giving Effective Feedback, Physician Communication, Setting Expectations & Enhancing Team Effectiveness, Leadership Skills for Senior Residents and Leadership Challenges for Chief Residents.
Stress management and impairment management for physicians in training is required of all PGY-I residents and is presented by the Office of Graduate Medical Education.
This is a lecture series presented by the Office of Graduate Medical Education that covers a broad range of issues including: contracting, patient and professional boundaries, patient safety, medical errors, medical legal issues, financial planning and debt management and health care systems among others. Many of these topics are mandatory for residents.
Ethical lectures sponsored by the Department of Surgery which are given 2 to 3 times annually and covers a wide range of ethical issues including patient confidentiality, truth-telling and communication, avoidance of medical malpractice, professional obligations, end-of-life issues, resource allocation, and informed consent. It is specifically oriented to surgical treatment.
A nationally recognized leader in urology is invited to the Southern Illinois University School of Medicine at least once each year. Visiting professors are selected on the basis of their regional and national reputation as well as their teaching ability. They are also selected on the basis of their background in urologic research and areas of special interest. Usually, these guests are residency directors or chairmen of other academic urology programs. They spend at least two days at our institution and participate in regularly scheduled conferences and individual discussion sessions. This is intended to allow a free interchange of ideas and case discussions by the resident staff. In addition, conference time is set aside so that the resident staff in urology may have an opportunity to present cases and discuss various topics in urology. The visiting professor also makes a formal presentation at the Surgical Grand Rounds with the entire surgical staff in attendance. In addition to the formal presentations, during each guest professor's visit, an evening program is provided to enhance the academic experience. Occasionally, they will be allowed to operate with the residents.


Resident rotations
Residents will rotate through SIU clinical service in 2-month (PGY-2&3/Uro-1&2 residents) and 3-month (PGY-4/Uro-3) intervals. The SIU service is responsible for participating in cases/clinics and managing the patients of the SIU attending urologist. One day per week, the adjunct faculty are also covered by the SIU service.
The areas of urology encompassed by the SIU service include:
- General urology
- Minimally invasive surgery (conventional laparoscopy, robotic-assisted laparoscopy and endourology)
- Oncology
- Andrology/male infertility/male incontinence
- Research
Example two-service model
- Uro-4 - chief resident-no service assignment
- Uro-3 - 3 mos/service; rotate attending for clinic
- Uro-2 - 2 mos/service; rotate attending for clinic
- Uro-1 - 2 mos/service; rotate attending for clinic
| July | Aug | Sept | Oct | Nov | Dec | Jan | Feb | Mar | Apr | May | June | |
|
SIU |
U3 | U3 | U3 | U3 | U3 | U3 | U3 | U3 | U3 | U3 | U3 | U3 |
| U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | |
| U1 | U1 | U1 | U1 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | U2 | |
| U1 | U1 | U1 | U1 | U1 | U1 | U1 | U1 | U1 | U1 | U1 | U1 |

