High Risk, High Reward
Rare antibody requires specialized care for pregnant mother
Aspects Volume 38 No. 3
Written by Rebecca Budde • Photography by Jason Johnson
Image Caption: McKenzie Sargent and her fourth child, Bryar, 5 months, who had the same life-threatening complications at birth as his older sister. Braylee, 3, Carter, 8, and Shaylon, 11, play in the background.
At only 10 days old, Braylee Sargent underwent a blood exchange transfusion, replacing approximately 80 percent of her blood volume in order to save her life. "It was a very long 10 days in a hospital room away from our other two children at home in Quincy," Braylee’s mother, McKenzie, says. "We hung on to every lab draw result."
Braylee was jaundiced and antibodies were attacking her red blood cells. She was placed under phototherapy lights, which help the jaundice by bringing the bilirubin levels down. "Almost all babies get jaundice at some point," says Beau Batton, MD, associate professor and division chief of neonatology. "In this case it wasn’t just the physiological jaundice after birth, but the pathological disease process that we worried about. The breakdown of the red blood cells can be so aggressive and so quick that the baby can become anemic." If the baby is anemic for too long, it can cause heart failure, and prolonged high bilirubin levels can lead to brain injury and hearing loss.
McKenzie recalls that day being one of the lowest and scariest of her life. "Just the thought of it gives me chills," she says. "We kissed Braylee and stepped into the waiting room and prayed."
Braylee’s parents, Greg and McKenzie Sargent of Quincy, had no reason to think that McKenzie’s third pregnancy or the health of their third child would be any different from the first two. But at eight weeks pregnant with Braylee, McKenzie’s blood work showed that she had a rare antibody in her blood that could threaten the life of her unborn child. She needed the help of a physician specializing in high-risk pregnancies.
A team of SIU providers in the divisions of Maternal Fetal Medicine, Neonatology and Genetic Counseling helped the Sargents. Robert Abrams, MD, associate professor and chief of Maternal Fetal Medicine, took over McKenzie’s care and worked with SIU neonatologists to prepare for the possibility of an early delivery or complications that could arise from McKenzie’s unique situation.
The antibody in McKenzie’s blood is called anti-c. When a mother’s blood is Rh-negative and the fetus’s blood is Rh-positive and the fetus’s blood crosses into the mother’s blood, the mother becomes isoimmunized. The mother’s body reacts to the fetus’s blood as a foreign substance and creates antibodies against it. Most commonly this occurs during delivery; for McKenzie isoimmunization likely happened during the delivery of her second child, Carter, 8.
Once McKenzie’s body had the antibodies, her unborn children were in a precarious situation. If the antibodies crossed the placenta, the fetus could develop hemolytic anemia – the antibodies attack the fetus’s red blood cells at a more rapid rate than the body can replace them. Because the function of the red blood cells is to carry oxygen to the body, this condition can be fatal to the fetus. The condition requires regular blood tests and frequent monitoring by a maternal-fetal medicine physician like Dr. Abrams.
McKenzie was nervous for each appointment. "I set little goals for myself to keep my nerves settled," McKenzie says. "When I was seeing Dr. Abrams every two weeks, I’d tell him ‘I haven’t slept since I saw you two weeks ago.’" Physicians used to rely on an amniocentesis as a tool to diagnose fetal anemia, but current technology allows them to test non-invasively using ultrasound. Additionally, blood tests show the level of antibodies in the mother. If the titers are too high or the ultrasound shows anemia and it’s too early for delivery, the fetus will need to have an in-utero blood transfusion through the umbilical cord: a risky procedure, according to Dr. Abrams. "The risk of stillbirth is 1 percent, which is quite high; but fortunately we rarely have to do in-utero transfusions, and luckily McKenzie and the baby didn’t need one."
"We made it through most of the pregnancy without complication, until 37 weeks, and then my antibody titers went through the roof," McKenzie says. "I wasn’t ready. We didn’t think Braylee’s lungs were developed enough either, but there wasn’t a choice." Dr. Abrams induced an early labor, and Braylee was born at St. John’s Hospital on October 3, 2011. Three days after Braylee was born, she showed signs of jaundice and anemia as the antibodies began to attack her red blood cells. The Sargents waited for good news, but the test results showed no signs of improvement for baby Braylee.
While Dr. Abrams continued to care for McKenzie, the family met Daniel Batton, MD, now retired professor and division chief of neonatology and other SIU’s neonatologists, including Dr. Beau Batton, Daniel’s son. The physicians explained the process of the exchange transfusion to the Sargents. "Over the period of several hours, we take out the baby’s ‘bad blood’ and transfuse in donor blood that doesn’t have the antibodies," explains Dr. Beau Batton. Although the procedure is safe, it’s not without risks: approximately a 1 percent chance of death and 1 percent chance of intestinal problems.
The exchange transfusion worked for Braylee, and the couple left for Quincy the next day to bring Braylee home to meet her older brother and sister. "Once we got rid of the antibodies in the baby’s blood, she was cured," Dr. Batton says. "Fortunately, the procedure has become less common due to the rarity of Rh disease."
Thanks to the use of special immune globulins called RhoGAM®, Rh incompatibility issues are extremely rare in areas with access to good prenatal care, according to Dr. Abrams. RhoGAM® was commercialized in 1968; researchers estimate that approximately 10,000 babies died each year prior to RhoGAM®. "It’s probably one of the greate st medical achievements of the 1960s; it has saved a tremendous amount of babies’ lives," Dr. Abrams says.
st medical achievements of the 1960s; it has saved a tremendous amount of babies’ lives," Dr. Abrams says.
After Braylee was born, the Sargents discovered that despite the rarity of anti-c isoimmunization, their children would always be at risk. SIU genetic counselors helped Greg receive genetic testing, which showed that he was a carrier. "I’ve always wanted five children," McKenzie says. "It was really tough deciding if we would have more children after Braylee."
Shortly after Braylee was born, McKenzie began working for SIU Quincy Family Medicine. When the couple decided to have another child, they did so with confidence in the SIU physician team. "Knowing those who would be taking care of my baby made me relax a little and feel more at peace," McKenzie says. "Each of these doctors who took care of me and my babies are one of my own, and I knew we were in the best hands possible."
Dr. Abrams was immediately assigned to McKenzie’s care and saw her through to full-term. The Sargents began a familiar trip down memory lane when their son, Bryar, was born on December 8, 2014. This time, Dr. Beau Batton was in the NICU caring for the baby. "My guess is that they felt like it was déjà vu with Bryar. The courses were pretty similar, the NICU was the same and even the doctor’s last name was the same," he says. "A few days of phototherapy helped with the jaundice, but Bryar still needed an exchange transfusion."
The procedure worked for Bryar, and the Sargents again returned home with another bundle of joy to share with their other children. "During these two scariest times of our lives we were surrounded by an amazing team of angels."
Above Image Caption: Bryar and Braylee SargentOB-GYN, neonatology keep care close to home
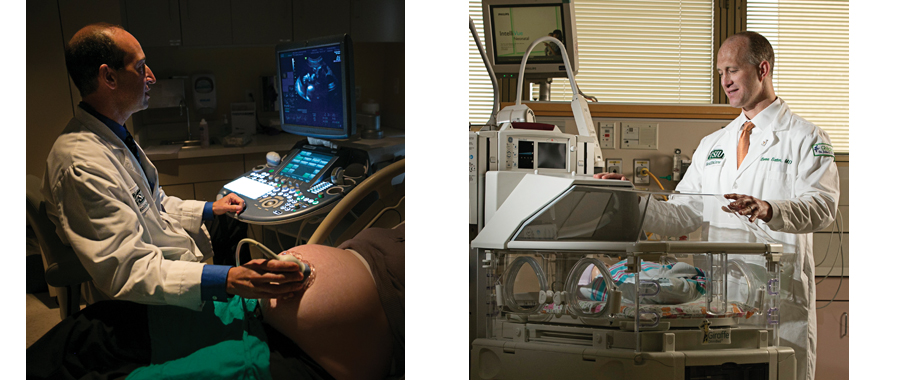
Image Right Caption: Dr. Beau Batton specializes in neonatal care.
As co-medical directors of the South Cental Perinatal Center at St. John’s Hospital, Dr. Abrams and Dr. Batton have developed a strong relationship between MFM and neonatology. The divisions hold weekly meetings to discuss patients who may deliv er early. "We also discuss any fetal issues we see in our outpatient clinic so that if they deliver in the middle of the night and the baby needs neonatal care, we have a list and know what the plan is," Dr. Abrams says. Dr. Batton then talks about the babies that were born that week. "We take care of the moms, but we don’t know what happens to the baby because they get whisked off to the NICU. Dr. Batton lets us know what happened so that if we see this condition again we have an idea of how things go."
er early. "We also discuss any fetal issues we see in our outpatient clinic so that if they deliver in the middle of the night and the baby needs neonatal care, we have a list and know what the plan is," Dr. Abrams says. Dr. Batton then talks about the babies that were born that week. "We take care of the moms, but we don’t know what happens to the baby because they get whisked off to the NICU. Dr. Batton lets us know what happened so that if we see this condition again we have an idea of how things go."
Dr. Abrams often sees the same patient for future pregnancies. "The knowledge we have from these meetings helps us be prepared for the next pregnancy."
For more than five years, Dr. Abrams has traveled to Quincy two to three times a month to help patients in need of a physician specializing in maternal and fetal medicine (MFM). SIU School of Medicine OB-GYNs and MFMs also provide care to patients in Taylorville, Decatur and Litchfield. They soon hope to expand to the Effingham area. "Some of the smaller hospitals in central and southern Illinois are closing, and there’s a great need for high-risk obstetrical care in our region," Dr. Abrams says. "We are the only MFM center to the southern tip of Illinois, and we cover all the way to the western border of Illinois and as far east as Champaign."
For women with high risk pregnancies, close-to-home medical care is vital. "For some of our patients, the long drive to Springfield just isn’t safe," Dr. Abrams says. "Unfortunately, we are seeing increasing rates of hypertension, diabetes and maternal mortality."
For the Sargent family, SIU’s commitment to serving the region meant fewer trips to Springfield, saving them money on fuel, child care and time off work. For McKenzie, who was already suffering from hypertension, the best benefit of Dr. Abrams caring for her in her hometown was less stress.
The plan for these high-risk pregnancies is to deliver the babies at St. John’s Women and Children’s Center, which has a Level III neonatal intensive care unit (NICU).
However, sometimes women who may not even be high risk go into preterm labor. "When a baby is premature, you want specialized care," Dr. Batton says. He collaborates with area physicians to be sure these babies receive the best possible care where they are. Approximately four times a year, he also travels to Quincy to consult on cases with physicians.
