Simulation & Skills Lab Curriculum
Advances in medical simulation technology have become a vital and exciting facet of the evolving way that EM residents undergo training. Simulation can provide training in a risk-free, supportive environment where the complex nuances of best-practice patient care can be identified, recreated, practiced and tested among different learners to ensure the highest levels of competency. At SIU, we strive to create common as well as unique crisis scenarios. Chaos can be created on demand and scenarios can mimic physiologic changes just as they would occur in real patients. We have a focus on utilizing unique and powerful learning opportunities in key competencies, including communication, teamwork, emergent conditions, and leadership, as well as in tasks that require well-practiced skills such as diagnostics and procedures.
Jason Kegg, MD
Director of Simulation
Procedures Skills Curriculum
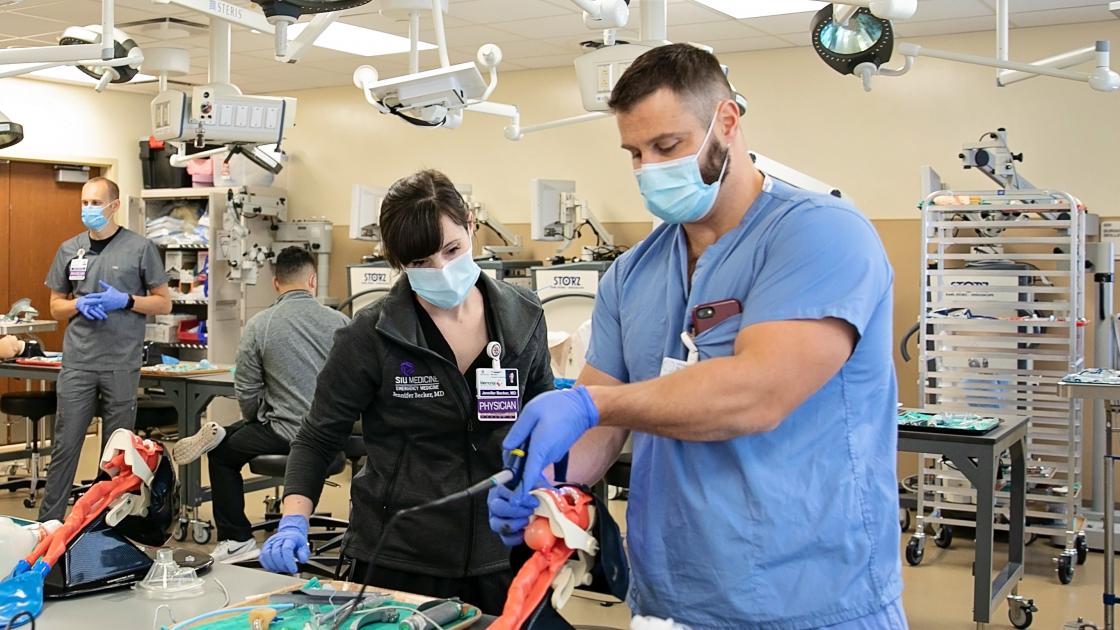
Procedures skills labs are held throughout the year integrated into Thursday conference. These labs were developed to provide technical instruction on performing procedures both common and uncommonly encountered in our field. Some examples of labs done in the past include airway management, advanced vascular access, cardiac pacing and pericardiocentesis, miscellaneous “centeses” and punctures, chest tube thoracostomy, open thoracotomy, peri-mortom c-section, fracture reduction/splinting, arthrocentesis, regional anesthesia, epistaxis control & HEENT procedures, and pediatric specific procedures. These skills labs take place in a state of the art skills lab at the Memorial Center for Learning and Innovations.
Simulation Curriculum
The simulation curriculum at SIU focuses on developing resident skill sets in emergency stabilization/resuscitation and interpersonal communication. These sessions concentrate on developing the medical knowledge needed to run a resuscitation, the psychomotor skills needed to apply complex bedside treatments, and the abilities to direct a multidisciplinary team through critical situations. Residents at our program have the luxury of performing these simulations in a state of the art simulation lab (link to MCLI?) with high-fidelity equipment. In addition, adjunct sessions concentrating on patient centered communication, vulnerable populations, and disclosing of adverse events are integrated to provide a well rounded experience. These sessions utilize well trained standardized patients to add to the realism and constructive feedback our learners receive while training with us. Residents at our program also perform the majority of their simulations with the nurses and techs they work with in our ED’s. This helps to forge deeper working relationships between our residents and their staff and provides a different point-of-view.
Simulated Milestone Assessment in Residency Training (SMART)
Once a year our program hosts a large scale simulation experience to assess both resident milestone progression and our curriculum in training the skill sets required of an emergency medicine physician. This large scale simulation helps to provide our faculty feedback on what needs added or changed regarding the core curriculum. In addition, it provides an opportunity to assess systems based practice training given these experiences involve collaboration and coordination with our EMS system coordinators, nursing staff and administration, and community partners. Most recent experiences have involved large scale mass casualty incidents and coordination of care through these difficult scenarios.
